 "How long does BPC-157 take to work?" is the most common question researchers ask after starting a protocol. The honest answer: it depends — and everything we know comes from animal models.
"How long does BPC-157 take to work?" is the most common question researchers ask after starting a protocol. The honest answer: it depends — and everything we know comes from animal models.
No human clinical trials have established BPC-157 timelines for any condition. What follows is extrapolated from published rat and mouse studies, where tissue repair endpoints were measured at specific time points. These animal timelines provide a framework, but they do not directly predict human outcomes.
This guide consolidates the available preclinical data into a realistic, week-by-week reference — organized by tissue type, with the caveats front and center.
Table of Contents
What to Expect: Managing Realistic Expectations
Before looking at timelines, three things need to be clear:
1. All data comes from animal models. The week-by-week timeline below is derived from rat studies where researchers sacrificed animals at specific intervals and examined tissue histologically. Rats metabolize faster, heal faster, and have different tissue architecture than humans. A "2-week result" in a rat study does not mean you should expect the same at 2 weeks (Sikiric et al., 2018).
2. Healing is not linear. Tissue repair follows a cascade — inflammation, proliferation, remodeling — and each phase has different timelines. BPC-157 appears to accelerate multiple phases simultaneously, but the subjective experience of improvement is often non-linear. Animal models show measurable changes (histology, biomechanics) before functional recovery catches up.
3. BPC-157 is not a miracle compound. It accelerates natural healing processes — it does not override biology. Severe injuries still take time. Chronic conditions that took years to develop will not resolve in days. The research shows faster healing, not instant healing.
With those caveats in mind, here's what the published data shows at each stage.
Week-by-Week Timeline from Animal Research
Week 1–2: Early Response Phase
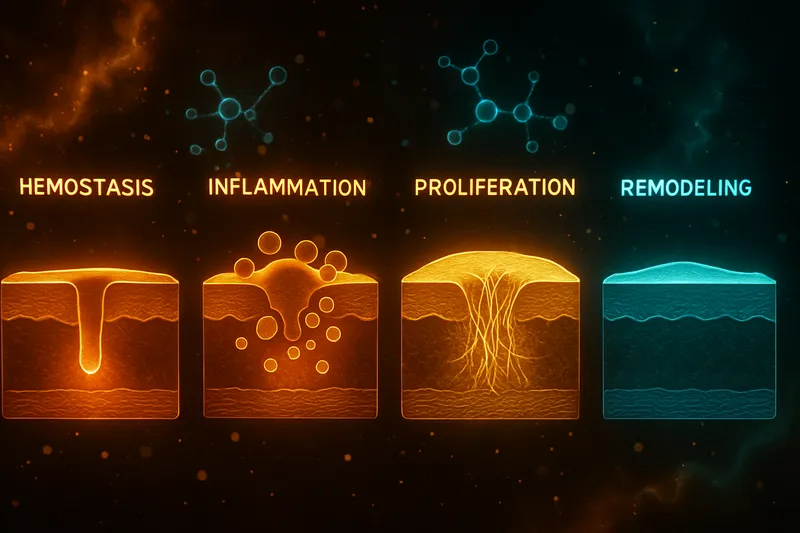
In the published literature, the first 1–2 weeks represent the acute healing window where BPC-157's effects are most rapidly observable in animal models.
What animal studies show at this stage:
- Gastric ulcers: Significant mucosal healing within 3–5 days. Sikiric et al. demonstrated near-complete healing of ethanol-induced and stress-induced gastric lesions in rats within the first week of daily BPC-157 administration (Sikiric et al., 1993).
- Inflammation: Measurable reduction in inflammatory markers and edema within 3–7 days across multiple tissue injury models (Seiwerth et al., 2018).
- Angiogenesis initiation: Early blood vessel formation begins, with increased VEGF expression detectable at injury sites by day 4–7 (Hsieh et al., 2017).
- Nerve injuries: In sciatic nerve transection models, early axonal sprouting is detectable histologically within the first 7–14 days (Gjurasin et al., 2010).
What this likely means in practice: The first two weeks are primarily about reducing inflammation and initiating repair cascades. Subjective improvement — if any — would most likely involve reduced pain signals and decreased swelling rather than structural tissue repair.
Week 3–4: Active Repair Phase
The 3–4 week mark is where the most significant structural changes are documented in animal studies. This is the window most researchers use for primary outcome measurement.
What animal studies show at this stage:
- Tendon healing: Chang et al. measured significantly improved tendon-to-bone junction integrity and collagen fiber organization at 4 weeks post-injury in BPC-157-treated rats versus controls (Chang et al., 2011).
- Ligament repair: MCL-transected rats showed measurably greater ligament tensile strength and improved collagen alignment at 4 weeks (Chang et al., 2014).
- Muscle recovery: Functional gait improvements in crush injury models, with histological evidence of reduced fibrosis and increased muscle fiber regeneration (Novinscak et al., 2008).
- GI healing: In colitis models, substantial reduction in mucosal damage scores and inflammatory infiltration by 3–4 weeks (Sikiric et al., 2003).
What this likely means in practice: This is where meaningful functional improvements would be expected — improved range of motion, reduced pain with activity, measurable GI symptom changes. The underlying tissue is undergoing active remodeling.
Week 5–8: Maturation Phase
Longer-duration animal studies show continued improvement through weeks 5–8, with tissue remodeling progressing toward more organized, functional architecture.
What animal studies show at this stage:
- Tendon biomechanics: Load-to-failure testing shows progressive strength gains beyond the 4-week mark, with BPC-157-treated tendons approaching normal tissue strength by 6–8 weeks (Staresinic et al., 2006).
- Bone healing: Enhanced callus formation and mineralization measurable at 6 weeks in pseudoarthrosis models (Krivic et al., 2006).
- Nerve regeneration: Improved electrophysiological parameters — motor nerve conduction velocity and compound muscle action potentials — measurable at 6–8 weeks post-transection (Gjurasin et al., 2010).
- Collagen remodeling: Transition from type III (scar) collagen to type I (functional) collagen continues through this window.
What this likely means in practice: Progressive functional improvement as tissue matures. This is the remodeling phase — the tissue exists but is being reorganized into functional architecture. Gains may feel slower subjectively even though structural improvements continue.
8+ Weeks: Long-Term Remodeling
Few published BPC-157 studies extend beyond 8 weeks, but the available data and general tissue biology suggest:
- Tendon and ligament remodeling continues for 3–6 months post-injury regardless of intervention
- BPC-157's primary contribution (angiogenesis, growth factor upregulation) is most impactful in the first 4–8 weeks
- Continued dosing beyond 8 weeks is not well-studied; most animal protocols conclude by this point
- Cycling patterns (4 weeks on, 2 weeks off) are commonly discussed but not validated in published research
Timeline by Use Case
Different tissues heal at different rates, and BPC-157 research reflects this. Here's a breakdown by injury type based on the published endpoints in animal models.
Gastrointestinal Healing
GI tissue has the fastest turnover rate in the body — the intestinal epithelium replaces itself every 3–5 days. BPC-157 research in GI models reflects this rapid baseline.
GI conditions are where oral BPC-157 administration is most supported by the research, given the peptide's gastric acid stability and direct contact with the target tissue.
Tendon & Ligament Repair
Tendons and ligaments are avascular — they heal slowly even under ideal conditions. BPC-157's angiogenic properties are particularly relevant here.
| Timeframe |
Observed Effect |
Source |
| 1–2 weeks |
Initial fibroblast migration, early angiogenesis |
Chang et al., 2011 |
| 3–4 weeks |
Improved collagen alignment, measurable tensile strength gains |
Chang et al., 2014 |
| 5–8 weeks |
Approaching normal biomechanical strength |
Staresinic et al., 2006 |
| 8–12 weeks |
Continued remodeling toward functional tissue |
General tissue biology |
Subcutaneous injection near the injury site is the most commonly used route in published tendon/ligament studies.
Muscle Injury
Muscle has better blood supply than tendon, so baseline healing is faster. BPC-157 appears to reduce fibrosis (scar tissue) while promoting functional muscle fiber regeneration.
Neurological Applications
Nerve tissue heals the slowest. Peripheral nerve regeneration occurs at roughly 1 mm/day, and central nervous system recovery is even more limited.
Nerve-related applications require the longest protocols in published research. Patience is essential.
Factors That Affect Results
Even in controlled animal studies, BPC-157 outcomes vary based on several factors. In real-world use, variability is even greater.
Dose and Frequency
Published research consistently uses daily dosing at 10 µg/kg in rats (human equivalent ~200–300 µg/day via allometric scaling). Studies using twice-daily dosing during acute phases show faster initial response compared to once-daily protocols. Underdosing is the most common reason for suboptimal outcomes. See our BPC-157 Dosing Guide for detailed protocol information.
Route of Administration
Route matters — especially for localized injuries. Subcutaneous injection near the injury site delivers higher local concentrations than systemic administration. Oral dosing is most effective for GI conditions and has demonstrated systemic effects in animal models, though bioavailability is lower than injection (Sikiric et al., 2018).
Injury Severity and Chronicity
Acute injuries respond faster than chronic conditions in animal models. A fresh tendon tear in a rat shows measurable improvement by week 2–3. A chronic degenerative condition has more damaged tissue to clear and remodel before functional improvement occurs. This is basic wound biology, not unique to BPC-157.
Stacking with Other Peptides
Combining BPC-157 with TB-500 is the most commonly referenced stack in the research community. The rationale: BPC-157 promotes angiogenesis and growth factor modulation while TB-500 drives actin remodeling and cell migration — complementary mechanisms for tissue repair. No published studies directly compare the combination to either peptide alone in the same model. For a detailed comparison, see our BPC-157 vs TB-500 analysis.
Individual Biology
Age, nutritional status, sleep quality, blood supply to the injury site, concurrent medications, and overall health status all affect tissue healing rates. BPC-157 accelerates existing repair mechanisms — it doesn't replace them. If the foundations of healing (nutrition, sleep, blood flow) are compromised, even an effective peptide will underperform.
How to Track Progress
Animal studies use histology, biomechanical testing, and imaging to measure BPC-157's effects. Researchers working with human subjects can track outcomes using several practical approaches.
Functional Assessments
- Range of motion testing — measured with a goniometer at consistent intervals (weekly)
- Pain scales — standardized VAS (visual analog scale) scores, recorded at the same time of day
- Strength testing — grip strength, manual muscle testing, or machine-based measurement
- Gait analysis — for lower extremity injuries, tracking stride length and symmetry
- GI symptom diaries — for gut-related applications, daily tracking of symptoms (bloating, pain, stool quality)
Biomarkers
- CRP (C-reactive protein) — systemic inflammation marker; expected to decrease as healing progresses
- ESR (erythrocyte sedimentation rate) — another inflammation indicator
- Calprotectin (fecal) — specific to intestinal inflammation; relevant for GI protocols
- Liver and kidney panels — safety monitoring, not outcome tracking
Imaging
- Ultrasound — useful for tracking tendon and ligament healing; can show collagen density changes
- MRI — gold standard for soft tissue assessment; 6–8 week intervals for comparison
- X-ray — relevant for bone healing protocols
Best Practices for Tracking
Document baseline measurements before starting any protocol. Record outcomes at consistent intervals — weekly for functional tests, monthly for imaging. Photograph visible injuries (swelling, bruising) under the same lighting conditions. Subjective improvement without objective measurement is unreliable.
Common Mistakes That Delay Results
Based on the published research and common protocol errors, several mistakes can compromise outcomes:
Underdosing
The most common issue. Published animal research uses 10 µg/kg daily — the allometric human equivalent is roughly 200–300 µg/day. Protocols using significantly lower doses may fall below the therapeutic threshold. The dose-response curve in animal studies shows activity across a wide range, but there is a floor below which effects diminish (Krivic et al., 2006).
Stopping Too Early
Tissue repair takes time. Tendon studies measure outcomes at 4–8 weeks. Nerve studies run 6–12 weeks. Stopping a protocol at 2 weeks because results aren't obvious means terminating during the proliferative phase — before the remodeling that produces functional improvement has occurred. If the published research runs 4–8 weeks, a protocol should match that duration at minimum.
Wrong Route for the Condition
Using oral BPC-157 for a knee tendon injury delivers lower local concentrations than subcutaneous injection near the injury. Conversely, injecting BPC-157 subcutaneously for a GI condition bypasses the direct mucosal contact that makes oral dosing effective for gut healing. Match the route to the target tissue.
Ignoring Foundational Healing Factors
BPC-157 enhances repair — it doesn't replace the requirements for healing. Sleep deprivation, caloric restriction, chronic dehydration, ongoing tissue stress (continuing to train through an injury), and smoking all impair healing through mechanisms BPC-157 cannot fully compensate for.
Poor Peptide Quality
Research-grade BPC-157 used in published studies has verified purity (>95% via HPLC). Products without third-party testing may contain degraded peptide, incorrect sequences, or contaminants. Purity directly affects bioactivity.
When BPC-157 May Not Work
BPC-157 is not effective for every condition. Understanding its limitations is as important as understanding its potential.
- Complete structural disruptions requiring surgery — a fully ruptured ACL or severed tendon needs surgical reconnection. BPC-157 may support healing post-surgery, but it cannot reattach completely separated tissues.
- Active infections — BPC-157 is not an antimicrobial. If an injury is infected, the infection must be treated first. For immune-modulating peptides, see LL-37 or Thymosin Alpha-1.
- Advanced degenerative conditions — severely degenerated cartilage or end-stage joint disease involves tissue that may be beyond repair acceleration. BPC-157 promotes healing of damaged tissue, not regeneration of tissue that no longer exists.
- Cancer-related tissue damage — BPC-157's angiogenic properties are a theoretical concern in the context of existing tumors. While no study has shown BPC-157 promoting tumor growth, its VEGF-upregulating mechanism warrants caution (Sikiric et al., 2014).
- Conditions requiring immune suppression — BPC-157 is not an immunosuppressant. Autoimmune conditions requiring immune downregulation may not respond to BPC-157's repair-focused mechanism.
- Unrealistic timelines — if someone expects a chronic 5-year tendinopathy to resolve in 1 week, BPC-157 will "not work" by that measure. The issue is the expectation, not the peptide.
Frequently Asked Questions
How fast does BPC-157 work?
In animal models, the fastest measurable effects occur in GI tissue — gastric ulcer healing within 3–5 days. Musculoskeletal effects are typically measured at 2–4 week intervals, with significant differences versus controls appearing by week 3–4. Nerve recovery studies run 6–12 weeks. All of these timelines are from animal research and may not directly apply to humans (Sikiric et al., 1993).
When will I feel a difference?
This guide intentionally avoids predicting subjective human experiences because no controlled human data exists. What can be said: animal studies show measurable tissue changes beginning in the first 1–2 weeks, with the most significant structural improvements at 3–6 weeks. Subjective human perception of improvement likely lags behind histological tissue changes.
Is 2 weeks enough time for BPC-157?
For GI healing, 2 weeks may be sufficient based on published animal data showing rapid mucosal repair. For tendon, ligament, or nerve conditions, 2 weeks is almost certainly too short — published studies measure primary outcomes at 4–8 weeks minimum. Stopping at 2 weeks means ending the protocol during the early repair phase.
Should I take BPC-157 once or twice daily?
Published animal research predominantly uses once-daily dosing, though some acute-phase protocols use twice-daily administration. Twice-daily dosing during the first 1–2 weeks followed by once-daily dosing is a commonly described approach in the research community. See our BPC-157 Dosing Guide for detailed frequency information.
Can I stack BPC-157 with TB-500 for faster results?
BPC-157 and TB-500 work through complementary mechanisms — BPC-157 via growth factor modulation and TB-500 via actin remodeling. The combination is widely referenced but no published study has directly compared the stack against either peptide alone. The theoretical basis for combining them is sound; the evidence for synergistic acceleration is anecdotal. See our BPC-157 vs TB-500 comparison.
What if I don't see results after 4 weeks?
First, verify: is the dose adequate (200–300 µg/day minimum based on allometric scaling)? Is the route matched to the target tissue? Is peptide quality confirmed via third-party testing? Are foundational healing factors (sleep, nutrition, avoiding re-injury) addressed? If all boxes check and 4 weeks produces no measurable change, the condition may not respond to BPC-157, or the injury may require a different intervention.
Does BPC-157 work for chronic injuries?
Animal models predominantly study acute injuries. However, BPC-157's mechanisms — angiogenesis, growth factor upregulation, inflammation modulation — are relevant to chronic conditions where healing has stalled. Chronic injuries may require longer protocol durations (8–12+ weeks) and may respond more slowly than acute injuries. No published timeline data exists specifically for chronic injury models.
Do results last after stopping BPC-157?
BPC-157 accelerates tissue repair — the healed tissue itself persists after the peptide is discontinued. Animal studies measure outcomes after treatment cessation and show maintained structural improvements. The tissue that was repaired doesn't "un-heal." However, the underlying condition that caused the injury (biomechanics, training load, systemic inflammation) still needs to be addressed to prevent recurrence.
References
-
Sikiric P, et al. "The pharmacological properties of the novel peptide BPC 157 (PL-10)." Inflammopharmacology. 1993;1(1):1-13. PubMed
-
Sikiric P, et al. "Therapy effect of antiulcer agents on new chronic cytoprotection model." J Physiol Paris. 2003;97(4-6):465-74. PubMed
-
Sikiric P, et al. "Stable gastric pentadecapeptide BPC 157-NO-system relation." Curr Pharm Des. 2018;24(18):1956-1969. PubMed
-
Seiwerth S, et al. "BPC 157 and Standard Angiogenic Growth Factors. Gastrointestinal Tract Healing, Lessons from Tendon, Ligament, Muscle and Bone Healing." Curr Pharm Des. 2018;24(18):1972-1989. PubMed
-
Chang CH, et al. "The promoting effect of pentadecapeptide BPC 157 on tendon healing involves tendon outgrowth, cell survival, and cell migration." J Appl Physiol. 2011;110(3):774-80. PubMed
This article is for educational and research purposes only. It is not medical advice. BPC-157 is not approved by the FDA for human use. All timelines described are extrapolated from animal research — no human clinical trials have established therapeutic timelines for BPC-157.
 "How long does BPC-157 take to work?" is the most common question researchers ask after starting a protocol. The honest answer: it depends — and everything we know comes from animal models.
"How long does BPC-157 take to work?" is the most common question researchers ask after starting a protocol. The honest answer: it depends — and everything we know comes from animal models.
