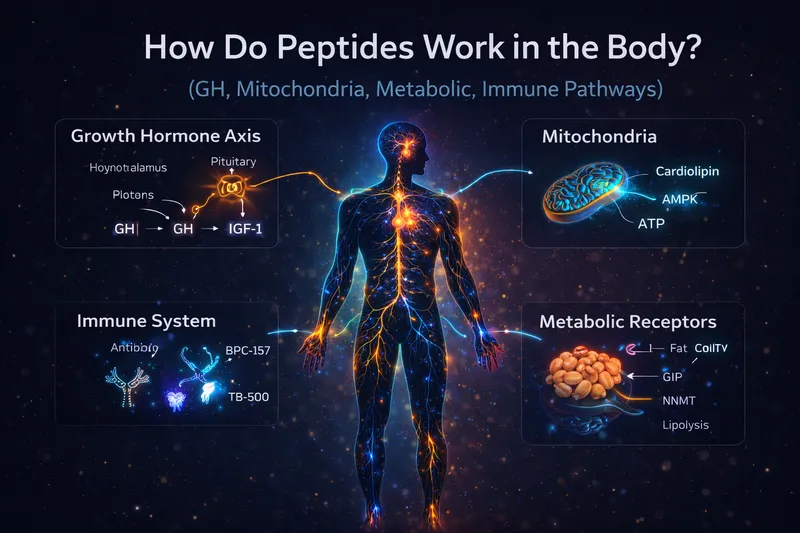
Peptides are short chains of amino acids that act as signaling molecules—chemical messengers that tell specific tissues in the body what to do. Unlike hormones (which impact many organs at once), peptides tend to be more targeted, binding to specific receptors and triggering precise biological effects.
Modern research has shown that peptides influence growth hormone signaling, mitochondrial function, fat metabolism, inflammation, and immune activation—but each category works through very different mechanisms.
Below is the most scientifically accurate breakdown available, with citations from PubMed, NIH, and peer-reviewed journals.
1. Growth Hormone Pathway Peptides
CJC-1295, Ipamorelin, GHRP-2/GHRP-6, Sermorelin
These peptides activate the GH axis, which has three main components:
- Hypothalamus → releases GHRH (Growth Hormone Releasing Hormone)
- Pituitary → releases GH (Growth Hormone) into circulation
- Liver → produces IGF-1 (Insulin-like Growth Factor 1) in response to GH
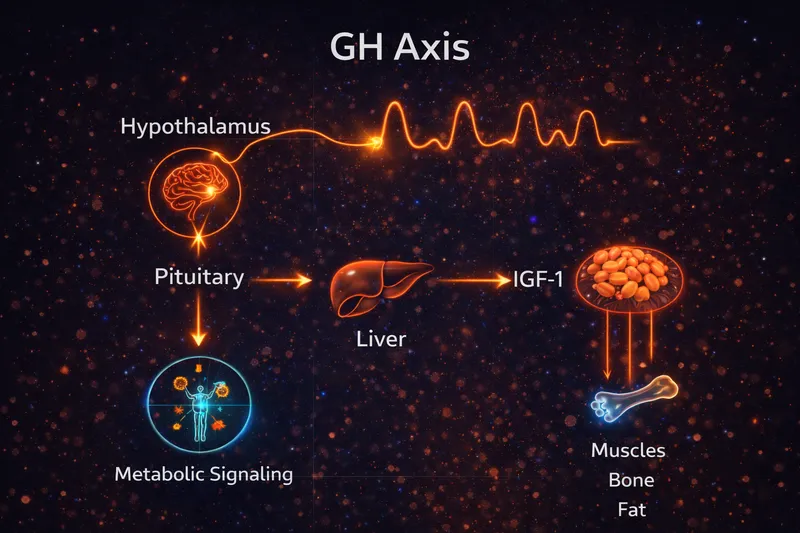
Why the GH Axis Matters
Growth hormone doesn't just affect growth—it regulates body composition, muscle protein synthesis, fat metabolism, bone density, and cellular repair throughout life. GH secretion naturally declines about 14% per decade after age 30, contributing to age-related muscle loss, increased fat storage, and slower recovery.
Source:
Unlike synthetic GH injections (which deliver a flat, unnatural dose), GH-releasing peptides work with your body's natural pulsatile rhythm—amplifying the pulses you already produce rather than replacing them.
They bind to GHRH receptors (GHRH-R) on somatotroph cells in the anterior pituitary, increasing the amplitude of natural GH pulses.
How GHRH signaling works:
- GHRH binds to its G-protein coupled receptor on pituitary cells
- This activates adenylyl cyclase, increasing cAMP levels
- cAMP triggers protein kinase A (PKA) activation
- PKA opens calcium channels and promotes GH gene transcription
- GH is released in a pulse that lasts 1-2 hours
📌 Key mechanism: GHRH peptides prolong the natural GH pulse, not override it. This preserves the body's feedback systems and avoids receptor desensitization.
CJC-1295 is modified with a Drug Affinity Complex (DAC) that extends its half-life to 6-8 days by binding to albumin, allowing for less frequent dosing.
Sources:
GHRPs bind to the Growth Hormone Secretagogue Receptor (GHSR-1a), also known as the ghrelin receptor. This is a completely different pathway from GHRH.
How ghrelin receptor signaling works:
- GHRP binds to GHSR-1a on pituitary somatotrophs
- This activates phospholipase C (PLC) via Gq proteins
- PLC generates IP3 and DAG, releasing calcium from intracellular stores
- The calcium surge triggers immediate GH release
- Additionally, GHRPs suppress somatostatin (the GH-inhibiting hormone)
Key differences between GHRPs:
| Peptide |
GH Release |
Cortisol |
Prolactin |
Appetite |
| Ipamorelin |
Strong |
Minimal |
Minimal |
Low |
| GHRP-2 |
Very Strong |
Moderate |
Moderate |
Moderate |
| GHRP-6 |
Strong |
Moderate |
Moderate |
High |
| Hexarelin |
Very Strong |
Higher |
Higher |
Moderate |
Why Ipamorelin is preferred: It selectively releases GH without significantly raising cortisol or prolactin, making it the "cleanest" GHRP for research.
Sources:
C. Combined Action (The Synergy Effect)
When GHRH + GHRP are used together (ex: CJC-1295 + Ipamorelin), something remarkable happens—the GH release isn't just additive, it's synergistic.
Why synergy occurs:
- GHRH increases the amount of GH released per pulse
- GHRP increases the frequency of GH pulses AND suppresses somatostatin
- Together, they amplify each other's effects by 3-10x compared to either alone
The resulting GH pulse:
- Higher amplitude (bigger peaks)
- Longer lasting (extended duration)
- More physiologic than synthetic GH injection
- Preserves natural feedback loops
This is why the CJC-1295 + Ipamorelin combination has become the most researched GH peptide stack.
Sources:
2. Mitochondrial Peptides
MOTS-c, SS-31, Humanin, Epitalon
These peptides originate from mitochondrial DNA (mtDNA)—a huge breakthrough in aging and metabolic science.

Why Mitochondrial-Derived Peptides Matter
Unlike nuclear DNA, mitochondria have their own small genome inherited exclusively from your mother. Scientists recently discovered that mtDNA doesn't just encode proteins for energy production—it also produces small signaling peptides called MDPs (Mitochondrial-Derived Peptides).
This discovery changed how we understand cellular aging. MDPs act as retrograde signals—messages sent from mitochondria to the rest of the cell and body, communicating metabolic status and stress levels.
Key insight: When mitochondria are stressed or dysfunctional (as happens with aging), MDP production changes. Restoring these peptides may help reverse age-related metabolic decline.
How MDPs Signal:
- They bind to receptors on cell surfaces and inside cells
- They activate protective pathways like AMPK (energy sensing) and reduce mTOR (growth/aging)
- They cross the blood-brain barrier, affecting both peripheral tissues and the brain
- They improve insulin sensitivity and reduce inflammatory markers
Source:
MOTS-c increases AMPK activation, which enhances:
- Cellular energy production
- Glucose utilization
- Stress resistance
- Exercise performance
Source:
B. SS-31 (Elamipretide)
SS-31 targets cardiolipin, stabilizing mitochondrial membranes and improving ATP output.
Benefits shown in human trials:
- Improved muscle energetics
- Reduced oxidative stress
- Potential reversal of age-related mitochondrial dysfunction
Source:
Humanin protects cells through:
- Anti-apoptotic signaling
- Reduction of oxidative stress
- Improvement of insulin sensitivity
Source:
Shown to:
- Increase telomerase activity
- Improve sleep
- Modulate circadian rhythm
Source:
Semaglutide, Tirzepatide, AOD-9604, Tesofensine, 5-Amino-1MQ
Metabolic peptides work through multiple pathways to influence appetite, fat storage, and energy expenditure. Unlike stimulants that force metabolic changes, these peptides work with the body's natural regulatory systems.
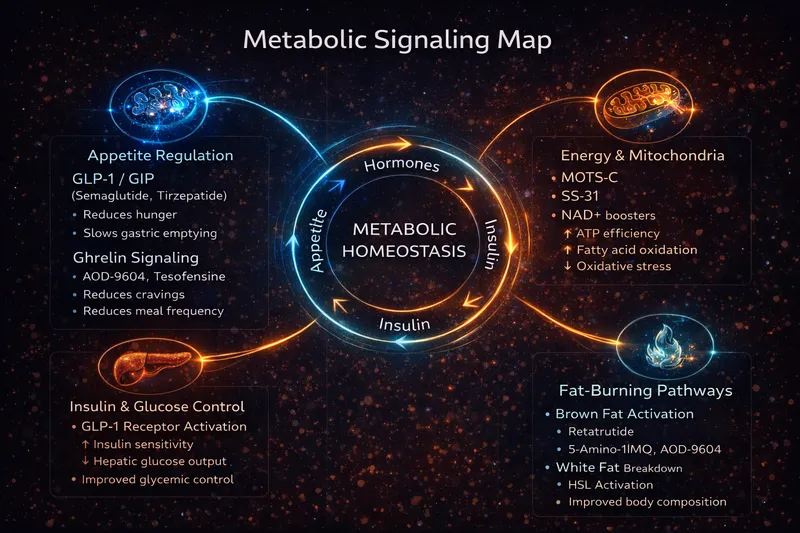
These are incretin mimetics—they mimic gut hormones that your body naturally releases after eating.
The Incretin System Explained:
When you eat, your gut releases two key hormones:
- GLP-1 (Glucagon-Like Peptide-1) — suppresses appetite, slows stomach emptying, increases insulin
- GIP (Glucose-dependent Insulinotropic Polypeptide) — enhances insulin release, affects fat storage
Naturally, these hormones are degraded within minutes by DPP-4 enzymes. Semaglutide and tirzepatide are engineered to resist this degradation, lasting days instead of minutes.
How GLP-1 reduces appetite:
- GLP-1 receptors exist in the hypothalamus (brain's appetite center)
- Activation creates feelings of fullness and satiety
- Gastric emptying slows, keeping food in the stomach longer
- Reward-related food cravings decrease
- Blood sugar spikes are blunted through improved insulin timing
Sources:
Semaglutide activates GLP-1 receptors with 94% homology to native GLP-1, but with a half-life of ~7 days (vs minutes for natural GLP-1). This allows once-weekly dosing.
Clinical results:
- STEP trials showed 15-17% average body weight loss
- Significant improvements in cardiovascular markers
- Reduced HbA1c in diabetic subjects
Sources:
Tirzepatide (Dual GLP-1/GIP Agonist)
Tirzepatide is a "twincretin"—it activates both GLP-1 and GIP receptors simultaneously. This dual action produces greater metabolic benefits than GLP-1 alone.
Why dual agonism matters:
- GIP receptors in fat tissue may improve fat metabolism
- Combined signaling creates stronger insulin response
- SURMOUNT trials showed up to 22.5% weight loss (vs 15% for semaglutide)
Sources:
AOD-9604 is a modified fragment of human growth hormone (amino acids 177-191). It retains GH's fat-burning properties while eliminating effects on blood sugar and IGF-1.
How AOD-9604 works:
- Binds to beta-3 adrenergic receptors on fat cells
- Activates hormone-sensitive lipase (HSL)
- Triggers lipolysis (fat breakdown) without affecting glucose metabolism
- Does not cause the insulin resistance associated with full GH
Key advantage: Unlike full GH, AOD-9604 doesn't raise IGF-1 levels, making it a "cleaner" option for fat metabolism research.
Sources:
5-Amino-1MQ works through a completely different mechanism—it inhibits NNMT (Nicotinamide N-methyltransferase), an enzyme that becomes overactive in obesity.
The NNMT-NAD⁺ Connection:
- NNMT consumes NAD⁺ (a critical cellular energy molecule)
- High NNMT activity depletes NAD⁺, reducing metabolic efficiency
- Blocking NNMT preserves NAD⁺ levels
- Higher NAD⁺ improves mitochondrial function and fat oxidation
- Studies show increased energy expenditure without stimulant effects
Why this matters for aging: NAD⁺ levels decline with age, contributing to metabolic slowdown. NNMT inhibition may help restore youthful metabolic function.
Sources:
4. Immune & Anti-Inflammatory Peptides
BPC-157, TB-500, LL-37, KPV, Thymosin Alpha-1
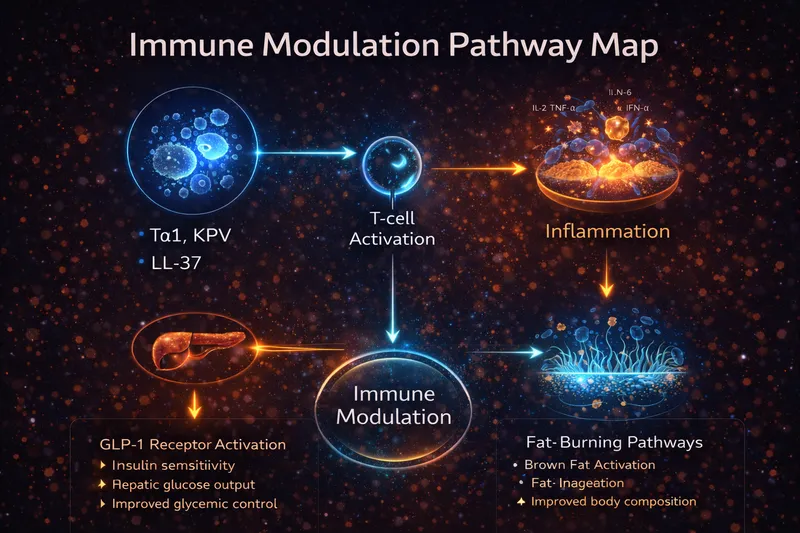
These peptides modulate the immune system and inflammatory response. Unlike immunosuppressants that broadly dampen immunity, these peptides tend to regulate immune function—calming overactive inflammation while supporting healthy immune responses.
BPC-157 (Body Protection Compound-157) is a 15-amino-acid peptide derived from human gastric juice. It's one of the most extensively studied healing peptides.
How BPC-157 promotes healing:
- Angiogenesis — Stimulates VEGF (vascular endothelial growth factor) to form new blood vessels
- Collagen synthesis — Increases fibroblast activity and collagen deposition
- Nitric oxide modulation — Regulates NO pathways, protecting blood vessel function
- Growth factor upregulation — Increases EGF, NGF, and other repair signals
- Cytoprotection — Protects cells from damage caused by NSAIDs, alcohol, and other toxins
Unique property: BPC-157 appears to work systemically—research shows it can accelerate healing in tissues distant from the administration site, suggesting it activates body-wide repair mechanisms.
Sources:
Thymosin Beta-4 is a 43-amino-acid peptide that's naturally present in nearly all human cells. TB-500 is a synthetic version of the active region.
How TB-500 works:
- Actin sequestration — TB-500 binds to G-actin monomers, regulating the actin cytoskeleton
- Cell migration — Actin regulation allows cells to move to injury sites faster
- Anti-inflammatory — Reduces inflammatory cytokines at injury sites
- Angiogenesis — Promotes new blood vessel formation for tissue repair
- Stem cell recruitment — May help mobilize stem cells to damaged areas
Key insight: The actin cytoskeleton is the "scaffolding" inside cells. By regulating actin, TB-500 helps cells migrate, divide, and reorganize—all critical for wound healing.
Sources:
LL-37 is the only human cathelicidin—a class of antimicrobial peptides that form part of the innate immune system. It's produced by immune cells, epithelial cells, and skin.
How LL-37 works:
- Direct antimicrobial action — Disrupts bacterial, viral, and fungal membranes
- Biofilm disruption — Breaks down protective biofilms that shield bacteria
- Immune cell recruitment — Acts as a chemokine, attracting immune cells to infection sites
- Inflammation modulation — Can both activate and resolve inflammation depending on context
- Wound healing — Promotes epithelial cell migration and angiogenesis
Dual role: LL-37 is unusual because it can fight pathogens directly while also signaling the immune system. This makes it a key bridge between innate and adaptive immunity.
Sources:
KPV is a tripeptide (Lys-Pro-Val) derived from alpha-MSH (alpha-melanocyte stimulating hormone). Despite being only 3 amino acids, it has powerful anti-inflammatory effects.
How KPV reduces inflammation:
- NF-κB inhibition — Blocks the master inflammatory transcription factor
- Cytokine reduction — Decreases IL-1β, IL-6, TNF-α production
- Gut barrier protection — Helps maintain intestinal epithelial integrity
- Melanocortin signaling — Activates MC1R receptors on immune cells
- No immunosuppression — Calms inflammation without broadly suppressing immunity
Why KPV is notable: It retains the anti-inflammatory properties of alpha-MSH without the tanning/pigmentation effects (those require the full molecule). This makes it useful for gut inflammation research.
Sources:
Thymosin Alpha-1 (Tα1) is a 28-amino-acid peptide originally isolated from thymus tissue. It's approved as a drug in over 35 countries for hepatitis and immune deficiency.
How Tα1 enhances immunity:
- T-cell maturation — Promotes differentiation of T-cells in the thymus
- Dendritic cell activation — Enhances antigen presentation
- NK cell activity — Increases natural killer cell function
- Cytokine balance — Shifts toward Th1 (antiviral) immune response
- Toll-like receptor signaling — Enhances pathogen recognition
Clinical applications: Tα1 (brand name Zadaxin) has been used clinically for:
- Chronic hepatitis B and C
- As an adjunct to cancer immunotherapy
- Immune reconstitution in immunocompromised patients
- Vaccine response enhancement
Sources:
Putting It All Together
Peptides represent a fundamentally different approach to biological signaling compared to traditional pharmaceuticals or even hormones.
Key Principles
1. Receptor Specificity
Each peptide binds to specific receptor types, triggering defined downstream effects. This is why peptides tend to have more targeted actions with fewer off-target effects.
2. Signaling Cascades
Peptides don't just flip a switch—they initiate cascades. A single receptor activation can trigger dozens of intracellular events, amplifying the initial signal.
3. Physiological Integration
Unlike synthetic drugs that override normal function, most peptides work within existing biological systems—amplifying natural processes rather than replacing them.
4. Context Dependency
Many peptides produce different effects depending on the tissue, the body's current state, and what other signals are present. This is why dosing and timing matter.
What Peptides Regulate
| System |
Peptide Examples |
Primary Mechanism |
| Growth Hormone |
CJC-1295, Ipamorelin |
GHRH/Ghrelin receptor activation |
| Mitochondrial |
MOTS-c, SS-31, Humanin |
MDP signaling, membrane stabilization |
| Metabolic |
Semaglutide, Tirzepatide |
GLP-1/GIP incretin pathways |
| Immune/Healing |
BPC-157, TB-500, LL-37 |
Growth factors, cytokine modulation |
The Bottom Line
Peptides are precision signals—not broad hormones. They work by:
- Binding specific receptors
- Triggering defined signaling cascades
- Amplifying or modulating natural biological processes
- Producing targeted effects in specific tissues
This precision is what makes peptides such an exciting area of research for conditions ranging from metabolic disease to tissue repair to healthy aging.
This article is for educational and research purposes only. It is not medical advice.




